For more information please visit our Educational Videos page.
Abdominal Aneurysms (AAA)
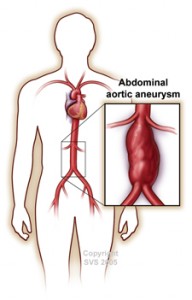
An aneurysm occurs when the walls of the aorta become weak and the diameter of the aorta increases. This is not an uncommon condition.
When the aneurysm affects the aorta in the abdomen (between the diaphragm and the pelvis) it is call a AAA. The size of AAA matters. Many different complications can occur including rupture with sudden death, complete blockage, or the aneurism can split the artery wall and cut off the blood flow to various parts of the body.
Who is at Risk?
Risk factors include smoking, high blood pressure, high cholesterol, emphysema, and in some cases, genetic factors. Men over the age of 60 who have one or more risk factors are most susceptible to abdominal aneurysms. Women are statically less likely than men to develop AAA.
Symptoms of an Aneurysm
Because aneurysms develop slowly, you may not be aware that you have one. However, if it ruptures, you may suddenly experience one or more of the symptoms below. Sudden discoloration in the lower extremities may signify the AAA has occluded.
Symptoms of a Ruptured Aneurysm
- Severe, sudden, or constant back or abdominal pain, which may also be felt in the groin, buttocks or legs
- Nausea and vomiting
- Rapid heartbeat
- Skin that feels cool and moist
- Shock
Tests and Treatments
An ultrasound or CT scan of the abdomen may detect the aneurysm. A routine physical exam often identify a AAA. In many cases, AAA are identified while a patient is undergoing tests for other problems. Depending on the size of the aneurysm, surgical aneurysm repair may be necessary to reduce the risk of a rupture. There are different options available in the treatment of AAA. Outcomes following repair are generally favorable.
Once ruptured, the outcome for patients is poor, but emergent treatment can be successful, and in some cases, patients will make a complete recovery.
Testing can be done in the PVA Vascular Lab.
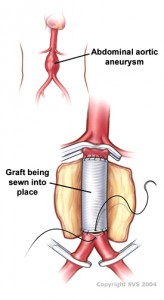
Open AAA